16 year-old Ananya Prasanna on the lesson from pharmaceutical scandal
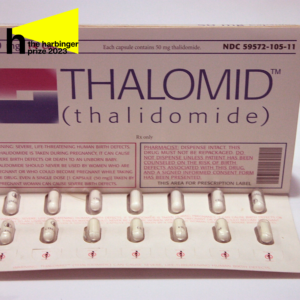
Contemporary packaging of Thalidomide has strict warnings - in 1950s, the drug was sold over the counter and marketed to pregnant women.
November 3, 2023
The Thalidomide scandal. A history of greed and neglect that shaped contemporary clinical trials
The year is 1961 and a family is excited to welcome a new baby boy into their home. He was, however, born with deformed limbs. Why? The answer is one word: Thalidomide.
Thalidomide is a sedative drug developed in the 1950s by a German pharmaceutical company Chemie Grünenthal GmbH.
The drug entered the market in 46 countries and after its distribution commenced in Britain by 1958, it quickly became a widely sought-after over-the-counter drug that ameliorates nausea and morning sickness – problems that are often faced by pregnant women.
Women using it were oblivious to the fact that their soon-to-be-born children would encounter wide-ranging birth defects, including deformed limbs and oesophageal malformations.
The drug bonded with specific proteins in the embryo’s body that control the formation of the extremities, causing malformations and preventing the limbs from further developing.
Article 19 of the Universal Declaration of Human Rights: “Everyone has the right to freedom of opinion and expression; this right includes freedom to hold opinions without interference and to seek, receive and impart information and ideas through any media and regardless of frontiers.”
This act was signed by the United Kingdom in 1948, a decade before Thalidomide was made available to the British population. Arguably, under this act, those using the drug should have been made aware of the potential consequences of using Thalidomide as soon as the pharmaceutical company, Grünenthal, were made aware of them.
Yet, even after hundreds of reports of infant death, Thalidomide’s association was denied by Grünenthal, effectively silencing the children and their families.
Consequences of Thalidomide are still refacing today, 70 years later, as it is now a drug used to treat leprosy. Although it comes with a strict warning not to be taken by pregnant women, unknowingly expectant women have taken the drug, which gave rise to a new wave of thalidomide babies. 70 years have passed, yet children are still dying.
One of the greatest mistakes was the nature of the clinical trials. Lacking placebos, a double-blind nature to the trial, and descriptions of the trial length, the trials Thalidomide underwent were crude and lacked scientific value.
The results should not have been used as evidence of Thalidomide’s efficacy and safety. Yet, when the drug was advertised, the results of these botched trials were used to persuade the public that Thalidomide was safe.
Without the use of a placebo (so giving some of the people in the trial a neutral substance) and double-blind trials (a procedure where neither the patient nor the doctor knows whether the tested substance was used), all those taking part in the trial knew that they take the tested substance which often results in patients feeling that the drug is more effective than it actually is.
The lack of disclosure of the length of the trial resulted in the fact that users could not discern whether there would be any long-term side effects of using it.
The most critical mistake was that the drug was not tested on pregnant women before the official release.
Therefore, there was no information whatsoever on whether and how Thalidomide affects a developing fetus.
Defendants of Thalidomide argued how in the 1950s, at the time of development, scientists were unaware that the effects of a drug could be passed through the placental barrier to directly impact the fetus and therefore it was not standard practice to test on expectant mothers before commercial release.
However, a drug with a similar sedative purpose that was developed earlier in the 1950s – Meprobamate – was tested against adverse effects on pregnant rats. It seems plausible that Thalidomide could have had similar tests.
This further supports the assumption that the purpose of Thalidomide’s trials was to enable the drug to be released as quickly as possible – a bid for profit, and not protection.
Why was it even possible for Grünenthal to deny any connection between Thalidomide and the deformation of the new-borns? The delay in establishing the connection is attributed to the fact that women whose children were born with characteristic deformations denied exposure to the drug because they did not take Thalidomide or Distaval (brands under which the substance was manufactured and sold in the UK) but an innocuous anti-flu treatment Grippex, which at the time contained Thalidomide.
In fact, with 37 treatments which contained Thalidomide around the globe, it took 5 years for the link to be confirmed.
It took until June of 1961 before an Australian doctor William McBride and his nursing team documented a definitive connection between the deformed babies born in their care and the usage of Thalidomide and alerted Distillers, one of the drug’s manufacturers.
Dr McBride was ignored and Distillers continued marketing campaigns claiming the drug was safe. Distillers claimed that Distaval [a brand name of Thalidomide] ‘can be given with complete safety to pregnant women and nursing mothers without adverse effect on mother or child.’
Later, the company claimed that they never received the calls from McBride – who continued to blow the whistle until late 1961 – or that the calls could have been taken by a junior member of staff who ignored their significance.
Michael Magazanik, an Australian lawyer, disputes Distillers’ claims. In ‘Silent Shock’, a book published in 2015, he interviewed Hubert Woodhouse, a salesman at Distillers’ Australian headquarters.
Woodhouse, who had signed an affidavit, revealed that Distillers’ top management had known there were strong concerns regarding Thalidomide’s safety by June 1961 and that he often joined the senior management after work for drinks, where Dr McBride’s warnings were often discussed.
Distillers was not the only company to ignore the warnings. German Grünenthal got reports of the malformations in 1959, 1960 and 1961, yet never investigated them.
In November 1961, McBride reported the concerns again, but this time with the support from German doctors. Finally, the drug was withdrawn from the market.
Even after Thalidomide’s was pulled back from distribution, the scandal continued, because the drug sat in many people’s medicine cabinets for months afterwards. In the UK, the government issued a formal warning against using it in May of 1962.
The delay in Thalidomide’s removal from the market and the official warning that the drug was unsafe meant that less children could have been saved.
Whether it be McBride’s ignored warnings, the Government’s late statement, or at the root of it, the inadmissible clinical trials, the Thalidomide scandal came as a result of malpractice from many parties and gave way to many lost and altered lives.
Article 5 of the aforementioned Universal Declaration of Human Rights states that ‘no one shall be subjected to torture or to cruel, inhuman or degrading treatment or punishment.’
Arguably, the ways in which the children of the Thalidomide scandal were treated were inhuman – they suffered as a result of clinical malpractice, mismanagement on the part of the companies, and the inaction of the authorities. Across the scandal’s tenure, not only was the health of mothers and children compromised, but their human rights.
Contemporarily, Thalidomide is being used to treat leprosy, AIDS and cancer. Although its circulation is restricted and regulated, it is important to consider the events of the past to ensure that the drug is safe for all who use it.
A number of precautions have been put in place: in the UK, women taking Thalidomide must take multiple forms of birth control to ensure they cannot become pregnant- all takers of Thalidomide undergo counselling to make sure that they understand all of the risks. With the UK’s rigorous systems in place to ensure drug safety, it is safe to say that the use of Thalidomide is highly regulated ensuring that history’s events will not repeat.
Thalidomide’s efficacy in treating leprosy is largely undisputed. However, in countries like Brazil, which has the second highest leprosy rate in the world, the more lax medical system has given rise to a new wave of Thalidomide children – with 30,000 new cases of leprosy a year and millions of pills being distributed it seems that the problem may be difficult to tackle.
Although Brazil has strict warnings on packaging, the common-place sharing of medicines has led to women unknowingly taking the drug without the necessary birth-control procedures – in which economic and educational inequalities play a part, as leprosy is a condition affecting predominantly the less privileged members of the Brazilian society.
Thalidomide was a tragedy that is often forgotten, but it shaped the strenuous clinical trials that take place today. Without the toll of Thalidomide, drug production may not be as safe as it is today.
The UK’s Committee on the Safety of Drugs was set up two years after Thalidomide was taken off the shelves. It stipulated strict requirements for testing on pregnant animals before introducing a drug, amongst other beneficial rulings. Since then, no prescription drug has had a similarly damaging effect on babies.
Thalidomide was certainly fatal for many and was a history of a clear violation of human rights. However, the lesson from this scandal saved lives for the future – and it is important that this lesson won’t be forgotten.




